Before we get into charting for fertility and monthly cycles, I want to start with the problems we face with our current conventional methods of contraception as well as the basics of what happens during each point in our monthly cycle.
Problems with birth control
Many forms of birth control may affect our chances later on when we would like to become pregnant. They may also inhibit our bodies’ natural hormone production.
We women, though only fertile a few days a month, put ourselves at great risk trying to prevent conception when we don’t feel ready for a baby. Blood clots, strokes, severe pelvic inflammatory disease, uterine scarring with IUDs, and urinary tract infections are just a few of many risks involved.
Along with other methods of birth control that use hormones to prevent conception, the Pill can cause major problems with how our bodies work. To begin with, they cause a flood of hormones into our system that have a cascading effect on our bodies’ own natural hormones. This in turn causes excess hormones to be excreted by the body; and if our liver isn’t working up to par, this excretion doesn’t always happen the way it should.
Over time, it may also cause our bodies to slow down production of hormones. When we stop taking these methods of birth control, our bodies may be severely lacking and must then figure out how to balance themselves again. Depending on the specifics of each body and how long you take hormonal birth control, this can take anywhere from weeks to years.
The Pill also uses your body’s stores of vitamin B (specifically B6), an essential nutrient your body uses to regulate menstrual cycles. Deficiencies in B6 can be linked to a progesterone imbalance as well as poor egg and sperm development and a short luteal phase.
There are also ethical ramifications when it comes to hormonal birth control. You see, the Pill works in three ways: stopping ovulation, decreasing the amount of cervical fluid, and preventing the uterine lining from thickening to allow for implantation. The problem here lies within the uterine lining. If conception does happen to occur, a fertilized egg is unable to attach to a thin uterine lining and passes through the body when menstruation occurs. For those that believe that life begins at conception, this can change the way one views hormonal contraception. I know it did for me.
(I must also note that most doctors do not support this theory of the abortive effect of birth control pills as one in particular stated that if hormones had allowed for the release of the egg, than it would also allow for implantation. So do your own research and come to your own conclusions. I was also told by an OB that if ovulation were to occur, that it’s reasonable to also believe that because an egg was released, that the corpus luteum will make enough progesterone to thicken the uterine lining. This is good news.)
The Natural Monthly Cycle
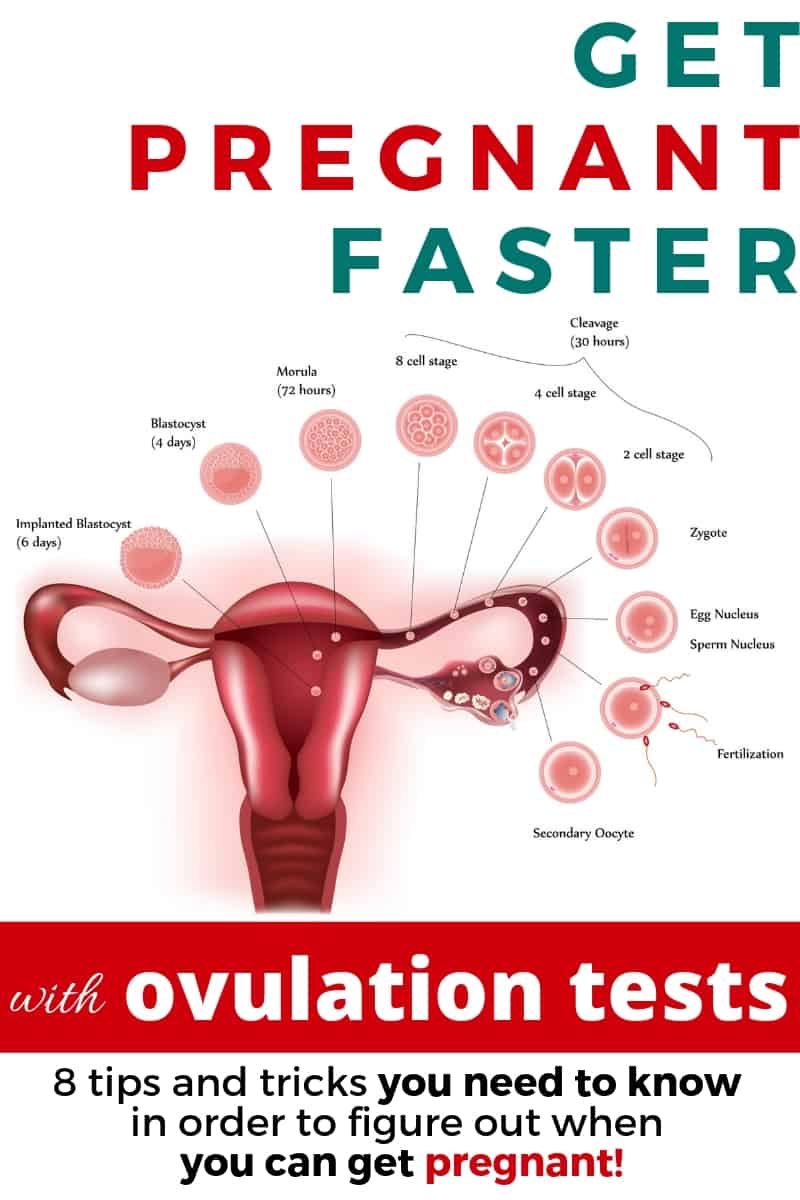
Each month a woman’s body produces a hormone called the Follicle Stimulating Hormone (or FSH), which helps to mature the 15-20 eggs that begin growing in her ovaries. Each egg is encased in its own follicle, and these follicles produce estrogen, which is necessary for ovulation to occur. The length of time it takes for an egg to mature varies a great deal from woman to woman. Some women’s eggs are ready in as little as 8 days, and for some it may take up to a month to reach the same maturity.
During this follicular phase, levels of estrogen also increase and cause the woman to start producing quality cervical fluid. Sperm can actually live about five days after ejaculation when a woman’s cervical fluid nourishes and feeds it. So it’s completely possible to get pregnant almost a week after intercourse! Once your body reaches its estrogen threshold and at least one egg is mature, the Lutenizing Hormone (LH) kicks into high gear and causes the egg to break through the wall of the follicle and begin its route down the fallopian tubes.
Now that the follicle is empty, it then collapses, becoming known as the corpus luteum, and starts producing progesterone. The corpus luteum only has a life of 12 to 16 days, and this life span is known as the “Luteal Phase.” This phase of the cycle happens to be a bit more important than what happens before ovulation because of the production of progesterone. The production of progesterone will now prevent all other eggs from being released and causes the uterine lining to thicken for implantation until the luteal phase is over.
To recap:
- Day one of the cycle (the first day of your period) starts the follicular (or estrogenic) phase and lengths can vary.
- From the day ovulation happens up until the last day before your period begins is the luteal phase.
- The luteal phase is not indefinite, meaning it has a finite life span of about 12 to 16 days.
- Once ovulation has occurred, the egg has a life span of about 24 hours (less time as we age and egg quality naturally goes down), after which it will either be reabsorbed into the body or be carried out by the menstrual flow if conception does not occur.
- If the sperm have had enough time to travel into the tubes and fertilization does occur (taking place within the fallopian tubes themselves), it usually happens within 12 hours post ovulation, as the quality of the egg begins to deteriorate over time.
- This fertilized egg will then be pulled into the uterus, and a few days to a week later this egg will finally reach the uterine lining and begins to burrow into it.
Now that the egg has burrowed into the uterine lining, it begins to release yet another hormone, called the Human Chorionic Gonadotropin—or HCG. This pregnancy hormone sends a signal back to the collapsed follicle (the corpus luteum) to stay alive past its normal 12 to 16 day life span. This happens so that it will continue to release progesterone, which in turn supports the pregnancy until the placenta can take over during the second trimester.
As women, we always know one thing about our cycle: when it begins. But how do we know when we ovulate? Check out the articles below for more information.
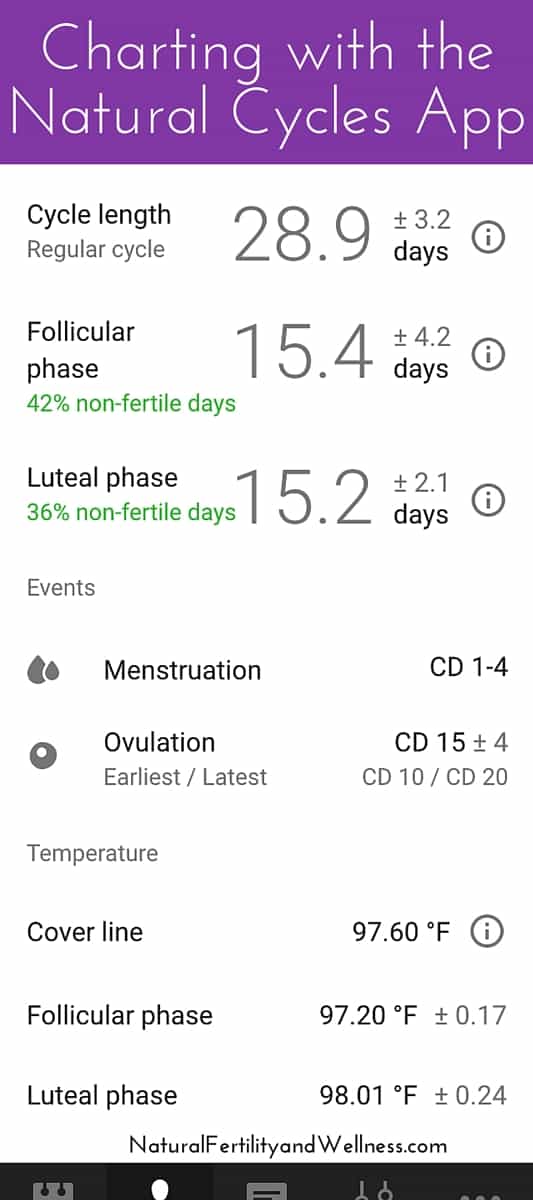
How to chart your temperature
Charting/checking cervical fluid
Charting/checking cervical changes
Secondary ovulation signs






 Breaking up with Weston A Price (the end of nutrition as I know it)
Breaking up with Weston A Price (the end of nutrition as I know it)
What about condoms?
@Lynn, while condoms do not interfere with hormones, they are bad for the environment because they don’t biodegrade. (Harder on the environment than another person’s whole lifelong impact? No. Still, it’s something to consider.)
The more serious concern about condoms is that they’re just not all that effective. For every 100 couples who use condoms as their only means of avoiding pregnancy for a year, 14 or 15 get pregnant. I think they are best used in combination with another method and/or to avoid disease.
The great thing about Fertility Awareness is that it always helps you to recognize when/if you are fertile, even if you are using artificial contraception. For example, I know someone who realized her pills weren’t working when she noticed fertile mucus–her doctor hadn’t mentioned that the antibiotic she was taking could interfere with contraceptive pills–and if she didn’t know what fertile mucus looks and feels like, she might have had an unwanted pregnancy then. So I think Fertility Awareness is a great idea for everyone!
Another plus is that it tells you when to expect your period. I have extremely long, irregular cycles, but I’m never caught by surprise now that I know how to recognize ovulation and count 2 weeks ahead.
As to the abortifacient effects of the pill, I would ask to doctor to read the package insert of the hormonal birth control. The companies themselves say that is one of the “lines of defense.” I hate how much politics is in medicine. *sigh*
It seems like NFP is a lot like birth. Women need to be encourage to trust their bodies and themselves!
@Emily, I wanted to clarify “that” as being thinning the lining of the uterus so the egg cannot implant.
As a teacher of natural family planning, I’m thrilled to see you approaching this from a standpoint of biology separate from religious issues. Although religious issues are important to me, I think they often cloud the picture: that hormonal b.c. is bad news for health & for environment, and that there’s a better way. Thanks!
I want to thank you for this article, I just wish I had read it ten years ago. Prior to my shift over to natural foods, medicines, and life choices, I assumed that whatever my doctor provided for me was helpful to my body. I initially went on the Pill not for contraceptive purposes, but to regulate my ‘abnormal’ period. After a few years on, few years off, few years on pattern, I finally started hearing the message from my body that it didn’t want me to keep taking these. So I came off of them, started noticing some improvement in symptoms I had been experiencing immediately, and then…. waited. And waited. And waited. For what? My period. It never came. It’s a year now, and I still haven’t restarted my cycle. I’m currently being treated with acupuncture and supplementation, and have been visiting a number of doctors for blood testing and exams, with no answers. Actually, not no answers- one answer seems to be, “Well, we’d like to run a test- one where we completely overwhelm your system for a period of (9?) days with progesterone, and then we run all sorts of tests on your hormone levels to see what’s going on.” I am starting to get desperate enough to find out what’s going on to want to do this, but I keep resisting, because I am CONVINCED that the introduction of outside hormones to my system is what has caused this problem in the first place. Please keep providing the information that you do; hopefully more women will see it and make changes in their health before they run in to a similar problem.
I’d also like to thank you for posting this article. Most women assume they know the “fertility basics”, but only once I started TTC did I realize how little we’re taught about our bodies and the reproductive system.
I was on the pill for almost 15 years, until my husband & I got married. I was always under the impression that BCP was relatively safe, as long as I wasn’t a smoker and didn’t suffer from any health problems. I learned too late that the REAL side effects could mean diminished fertilty during my reproductive years.
My husband & I have both been given a clean bill of health by our fertility specialist, and yet we’ve been trying unsuccessfully to conceive for more than two years now. In the last 3 months we’ve switched to mainly organic foods, and I have cut out dairy, grains, and sugar almost entirely. I’m hoping this will help alleviate the burden on my liver and “kick-start” my fertility.
In the meantime, I’ll be keeping an eye out for more natural fertility tips. Keep up the good work!
I apologize if this question has been asked somewhere else and I didn’t notice, but is it possible to have “fertile” cervical fluid without actually ovulating?
@Janelle, In some cases, yes. I’ve often heard many women state that their body “gears up”, trying to get the estrogen to spike high enough to cause ovulation (estrogen also causes more cervical fluid). If it doesn’t get high enough ovulation won’t happen, but they still had a day or so of fertile fluid.
Thank you for your reply. 🙂